Knee Replacement Surgery – What Is It? How Does It Work?
Knee replacement surgery is among the most efficient orthopedic procedures available today. Most patients report little or no knee discomfort, improved mobility, and overall quality of life.
“Learn more about knee replacement surgery, including its risks, benefits, recovery time, and cost.”
What is a Knee Replacement Surgery?
Knee replacement surgery is an option for people whose knees are severely damaged by arthritis. It involves replacing the damaged parts of the knee joint with artificial components that allow the patient to walk normally again.
Knee replacement, commonly known as knee arthroplasty or total knee replacement, is a surgical operation orthopedic surgeons use to reconstruct an arthritis-damaged knee.
During surgery, your surgeon will use metal and plastic parts to cap the ends of the bones that make up the knee joint along the kneecap.
Related Read: https://seniorcitizenwebsite.com/healthy-living-and-physical-wellness/
Who Needs Knee Replacement Surgery? Why?

This surgery is perfect for someone with severe arthritis or a serious knee injury. You may require this type of surgery if you have had an injury to your knee joint, such as a sports injury.
Osteoarthritis is when the cartilage between bones wears down, causing pain and stiffness. This arthritis usually affects older adults, although younger patients can also develop it. People who suffer from severe knee pain due to osteoarthritis often need knee surgery.
Because different types of arthritis often affect the knee joints, orthopedic surgeons have used knee replacement surgeries as a treatment for osteoarthritis since the 1970s.
Here are the different kinds of knee arthritis and how they affect the knee bone:
- Osteoarthritis, a degenerative joint condition mainly affecting middle-aged and older individuals, can destroy joint cartilage and adjacent knee bone.
- Rheumatoid arthritis causes synovial membrane inflammation and excess synovial fluid and can cause discomfort and stiffness.
- Traumatic arthritis, or arthritis caused by accident, can destroy the cartilage in the knee.
People with deformities such as bowed legs or ‘knock-knees’ may also require knee arthroplasty or knee replacement to restore the position of the knee.
The sole aim of arthroplasty is to repair damaged areas of the knee joint and reduce knee discomfort that you cannot manage with conventional physical therapy.
A video can explain it even better.
To totally grasp the concept of knee replacement surgery, let’s dive a bit into the knee anatomy.
Is a Knee Replacement a Major Operation?
A knee replacement is major surgery. This means your doctor will only recommend it if other treatments, such as physical therapy or steroid injections, haven’t helped reduce pain or increase your chances of having a healthy knee.
Anatomy of the Knee

The first thing to know is the knee is a joint. Joints are the places at which two or more bones meet. The majority of joints are movable, which allows the bones to move.
The knee comprises two long leg bones kept together by muscles, ligaments, and tendons. A layer of cartilage covers each bone end, absorbing shock and protecting the knee.
There are two groups of muscles in the knee that allows it to work perfectly – the quadriceps muscles and the hamstring muscles.
The quadriceps muscles (situated on the front of the thighs) straighten the legs.
The hamstring muscles (situated on the back of the thighs) help you bend the leg at the knee.
Present in the knee is also tendons. Tendons are thick connective tissue cords that link together muscles and bones.
Ligaments are elastic tissue bands that connect bones together. Some knee ligaments are there to provide stability and protection of the joints, while others limit the tibia’s (shin bone) forward and backward mobility.
The Types of Knee Replacement Surgery
There are five major types of knee replacement surgery. Depending on your orthopedic surgeon and depending on other conditions, like your age, health, and other results that state how much knee cartilage is damaged, you may require the following kinds of knee surgery:
Total Knee Replacement.
A total knee replacement surgery can also be referred to as Total Condylar Knee Arthroplasty.
In total knee replacements, your doctor will replace the entire knee joint with an artificial knee.
To determine if you require a total knee replacement surgery, your orthopedic surgeon must first assess your knee motion, stability, and strength.
To determine the extent of damage, most hip and knee surgeons will ask their clients a couple of questions, such as:
- Do you feel severe knee pain every time you engage in normal activities such as climbing stairs?
- Have you had a severe knee injury before?
- Do you feel pain in your leg muscles when you are walking?
- Do you experience difficulty getting in and out of chairs?
- Do you experience knee pain at rest? Etc.
Asides from these questions, your doctor will likely recommend a complete physical examination to see the extent of the damaged cartilage.
How is a Total Knee Replacement Surgery Performed?
The surgeon begins by making an incision (cut) in the knee and repositioning the patella (kneecap) to the side. If bone spurs (small bony growths) are present, which is common in osteoarthritis, your doctor will remove them.
The two menisci between the tibia and femur, the anterior cruciate ligament (ACL), and, sometimes, the posterior cruciate ligament (PCL), are removed.
In some knee replacements, the surgeon may decide to keep the PCL.
Then the surgeon cuts and removes cartilage and some bone from the upper portion of the tibia and lower regions of the femur during the major phase of the procedure.
The femoral parts that the doctor removes are two knobby protrusions known as the femoral condyles.
The tibia and femur are then capped with knee replacement implants (mostly metal) to form new joint surfaces. The new femoral component’s surface replicates the form of the original femoral condyles.
If the kneecap has already degenerated, the bottom surface may be removed and replaced with a polyethylene implant.
In the final step of total knee replacement surgery, the doctor repairs the various layers of tissue with dissolvable sutures. The skin incision is closed with surgical staples or sutures.
Once a bandage is wrapped around your knee, you will be taken into the recovery room.
In some cases, the surgeon may use robotic technologies during the operation.
In a sentence, total knee replacement is when your surgeon replaces the exteriors of the thigh bone and shin bone that connect to the knee.
Total knee replacement is the most common of all the different knee replacement surgeries.
Partial Knee Replacement
In this replacement knee joint procedure, your surgeon replaces only one compartment of your knee.
If your arthritis just affects one side of your knee, this surgery may be an option.
However, it is only appropriate for you if you have strong knee ligaments and the remainder of your knee cartilage is normal.
The incision your surgeon creates in a partial knee replacement is considerably smaller than what is used for total knee replacement.
For some people with knee osteoarthritis, a partial knee replacement is an excellent alternative to a total knee replacement.
So far, the injury in the knee joint is limited to a specific compartment of the knee; your doctor should be able to perform this surgery.
The purpose of this surgery is to replace only the damaged section of the knee cartilage with a prosthetic.
Previously, this surgery was reserved for elderly patients who participated in limited activities. But now, it is commonly performed on younger patients since recovery is faster and less painful.
- Patellofemoral Replacement.
This type of knee arthroplasty replaces the underside of the kneecap and the groove it rests in. This can be quite beneficial for persons suffering from persistent knee arthritis.
- Complex (or revision) Knee Replacement.
If you have severe arthritis or have previously had two or three knee replacement procedures and still need further surgery, this procedure knee replacement surgery may be necessary
- Cartilage Restoration
When there is only one region of damage or wear on the knee, your surgeon can replace this area with a live cartilage transplant or cells that develop into cartilage.
Risks of Knee Replacement Surgery
Knee arthroplasty, like any other procedure, has hazards. They are as follows:
- Blood clots in the lungs or leg veins
- Heart Attack
- Stroke
- Nerve Damage
- Infection:
An infected surgery site usually requires surgery to remove the artificial knee joint if it is a total knee replacement surgery. The same also goes for other types of knee surgery.
Your doctor will also prescribe antibiotics to kill the bacteria.
After the infection is cleared, the doctor will have to perform another surgery to install a new knee. - The ‘new knee’ can wear out.
A risk of total knee replacement surgery is the failure of the new knee joint.
Since you will use it daily, the wear will start telling on even the strongest metal and plastic knee replacement implant over time.
The risk is higher if you stress the knee joint with strenuous exercise or heavy weight lifting.
You should notify your doctor instantly if you notice any of the following.
- Fever of more than 100 degrees F (27.8c)
- Cold
- Drainage from the surgical site
- Chronic knee inflammation
- Increasing tenderness in the knee, swelling, and knee pain
How To Prepare For Knee Replacement Surgery
There are many things you can do before the surgery that will have a positive effect on the outcome. Here is a video that gives some tips and ideas.
How Long Does it Take to Recover from Knee Replacement Surgery?
Recovery time varies based on the individual and the type of surgery performed. However, the recovery time is shorter if you follow the hospital’s recommendations on how to care for your knee.
You may be given a switch on the surgical ward that allows you to self-administer pain medications at a safe pace to relieve pain. You may receive oxygen via a mask or tubing, depending on the situation. You will be offered a blood transfusion if necessary.
You’ll have a big dressing on your knee to protect the surgery site. Following surgery, a tube may be placed to drain blood from the surgery site and prevent it from pooling inside the incision.
The hospital staff will help you to get up from the bed and walk about as quickly as possible. Depending on your type of surgery, you, the nurses, or other care agents, will help you stand within 12-24 hours after the operation.
After this, you will have to walk with a frame or crutches, but after a week, you most likely be able to walk independently with a stick.
While you are still in the hospital, a physical therapist will come by to teach you exercises to strengthen your knee.
Usually, physical therapy begins the day after, or even on the same day as your operation (if there are no complications).
Physical therapy is important for you. It is equally as important to follow the instructions of your physical therapist to avoid the dislocation of your new joint.
It’s typical to feel discomfort initially while walking or exercising, and your legs and feet may be swollen.
However, you may be placed on a passive motion machine to regain mobility in your knee and leg. While you are in bed, this support will gradually move your knee. It helps to reduce swelling and enhance circulation by keeping your leg lifted.
All in all, you’ll probably spend between 2-3 days in the hospital.
It is vital to note that patients who had a total knee replacement surgery usually have a more extended hospital stay than those who have had other knee surgeries.
What You Can Do After Knee Replacement Surgery
Knee recovery affects everyday movement. See our senior mobility support tips for more
What is the Most Commonly Reported Problem after Knee Replacement Surgery?
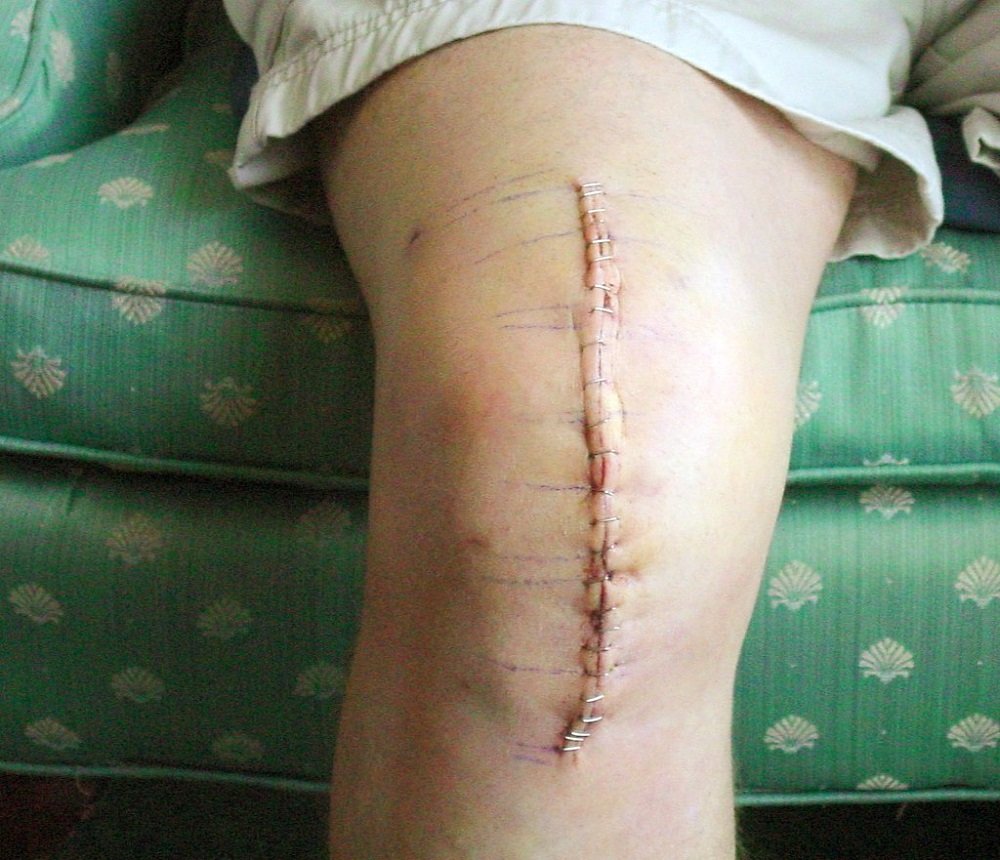
A stiff knee joint is one of the most commonly reported problems following knee replacement. These symptoms can frequently make regular activities difficult, such as sitting in a chair, climbing stairs, or getting out of a car.
Another commonly reported problem is hearing a clicking or clunking noise from the knee.
Usually, if you just hear the noise without feeling pain, it is not a problem. Still, report it to your healthcare provider to ensure there is nothing to worry about.
Because most knee replacements are comprised of metal and plastic, you may hear a clicking, clunking, or popping sound as the knee bends back and forth.
A more serious issue knee replacement patients commonly report, is the wearing out of implants.
Although the goal is for the knee replacement implant to last a lifetime, this is not always the case.
If the implant is beginning to wear out, your surgeon may recommend a revision knee replacement.
What is the Best Age to Have a Knee Replacement?
There is no such thing as the best age or worst age for knee replacement surgery. If it is difficult for you to sit, walk, or work without experiencing severe knee discomfort, you may be suitable for a knee replacement.
The most prevalent age group for knee replacement patients is between the ages of 50 and 70. However, with the increasing prevalence of early osteoarthritis and other joint disorders, numerous younger people may potentially be candidates for this surgery. Patients over 70 may also benefit significantly from the mobility and comfort that a prosthesis provides.
A patient under 45 is young, and having such a big operation so early in life is typically not advised.
Furthermore, younger folks are more active, which might cause the implant to wear out faster. In such circumstances, the patient may need a second knee replacement within 15 years of the first. The second operation is typically more difficult on the body than the first, and recovery can be difficult.
There is no set age restriction for knee replacement. You will be considered for surgery depending on various variables, including the severity of your symptoms and general health. If the advantages outweigh the dangers, your doctor may advise you to proceed with the operation.
Knee Replacement Surgery – Conclusion
Compare to hip replacement surgery this surgery will probably have you back up your feet faster.
After the surgery, you still have to look after your kneecap replacement. Here are some helpful tips to guide you through this:
- Continue taking any prescription painkillers or anti-inflammatories to help manage discomfort and swelling.
- Continue to use your walking aids, but try to gradually reduce your reliance on them as your leg feels stronger.
- Maintain your workouts and physical therapy to help avoid stiffness, but do not strain your knee.
- Do not sit crossing your legs for the first six weeks following your surgery.
- Keep your knee from turning. You can use a grabber tool to help.
- Outdoors, use supportive footwear.
- When sleeping, do not place a pillow beneath your knee since this might result in a permanently bent knee.
- Kneel on your operated knee only when your surgeon advises so.
- To minimize swelling, lift your leg when sitting and use an ice pack for 20 minutes every 3 or 4 hours.
You can resume most of your normal activities, such as shopping and minor housekeeping, within three to six weeks after surgery.
You can also drive after three weeks so far you can bend your knee far enough to ride in a car, have sufficient muscular control to use the brakes and accelerator, and are not currently on narcotic pain drugs.
Following your recovery, you can engage in low-impact activities such as walking, swimming, golfing, or bicycling. However, avoid high-impact activities such as running, skiing, tennis, and contact or leaping. Discuss your restrictions with your doctor.
Knee replacement relieves pain and provides greater mobility and a higher quality of life. Furthermore, most knee replacements are predicted to endure longer than 15 years.
Eddie Vandam
About the Author: Eddie Vandam
Eddie Vandam is a proud senior and retired internet marketer who now dedicates his time to helping others age well. As the voice behind the Senior Citizen Website, he shares practical advice on staying healthy, independent, and informed. From product reviews to wellness tips and hobbies that keep life interesting, Eddie writes with real-world experience and a passion for making senior life easier and more enjoyable.👉 Read more about Eddie Vandam.








